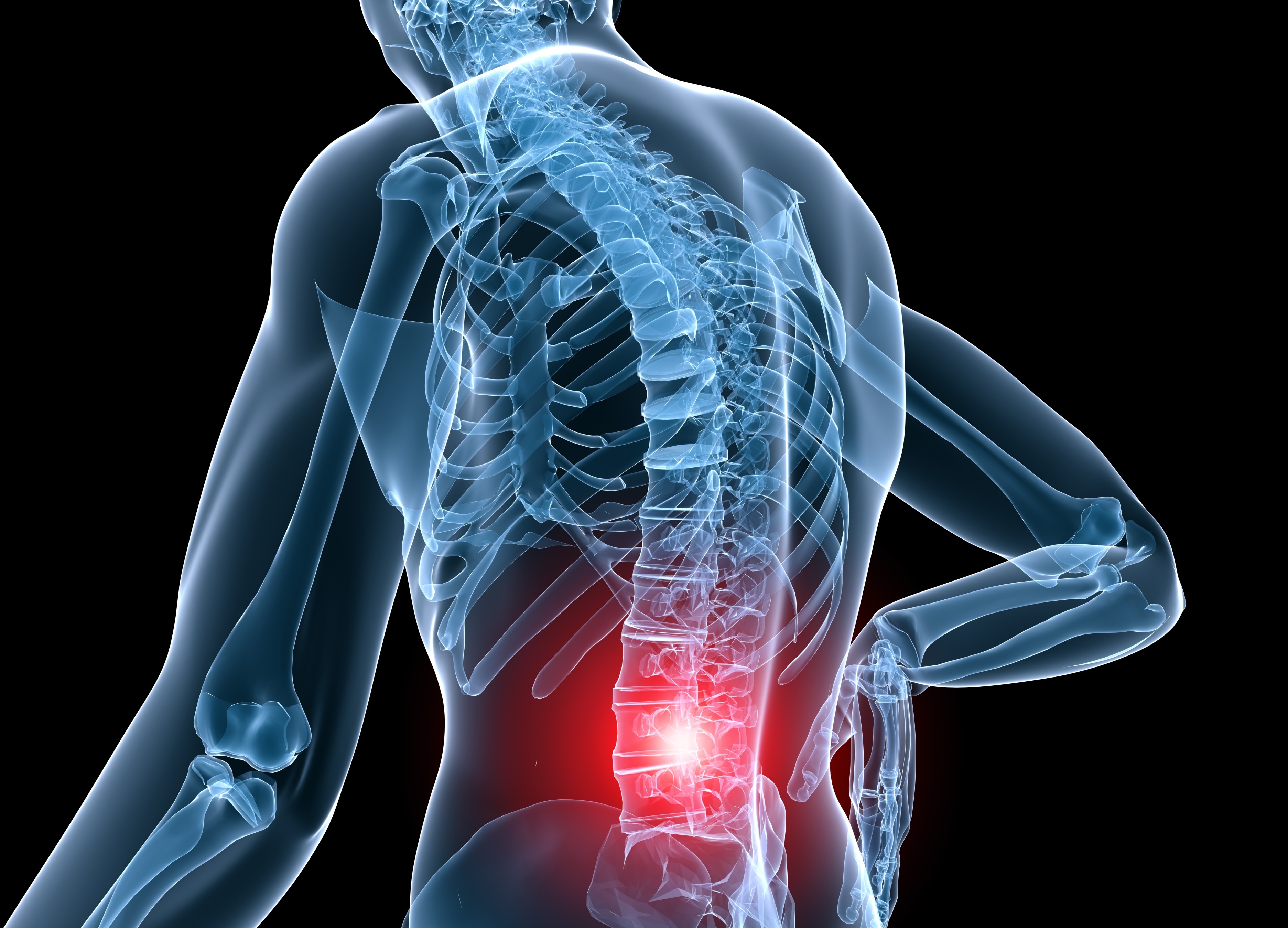
The ability to breath in (inspiration) and out (expiration) is driven by the pressure difference between the lungs and the atmosphere. This requires contraction and relaxation of the diaphragm and the muscles in the thorax. During normal relaxed breathing, contraction and relaxation of the diaphragm and the intercostals muscles (found between the ribs) cause most of the pressure changes that result in inspiration and expiration. The ability of the thoracic wall to stretch and recoil while under pressure influences the process of breathing. In normal inspiration an increase in the volume of the thoracic cavity is produced by the downward movement of the diaphragm and external intercostal muscles which move the ribs upward and outward, causing the rib cage to expand. The expiration in normal breathing is passive caused by the recoil resulting from the elasticity of the lungs. Additional muscles such as neck muscles are used during forced inspiration and abdominal and internal intercostals muscles are used during forced expiration. The respiratory rate is controlled by the respiratory centers located within the brain and the chemoreceptors present in the periphery. Although changes in pH levels and a large drop in blood oxygen levels can influence breathing, the major factor that stimulates the breathing rate is the concentration of carbon dioxide in the blood. The increase in breathing rate during exercise is thought to be influenced by the psychological, motor neuron and proprioceptor inputs.
In healthy subjects the diaphragm plays the dual role of spine-stabilization and respiration. During movements of the spine or extremity, the back extensors, diaphragm, pelvic floor and abdominal wall muscles activate synchronously. Diaphragm contributes to an important role in spinal stability through modulating the intra-abdominal pressure when the spinal stability is challenged. Although the diaphragm and abdominal muscles activate in opposition during respiration, a coordinated contraction of these muscles provide respiration and control of the spine simultaneously when in need co-ordinated by the central nervous system. It is described that dysfunction in one function, either respiration or spinal stabilization can negatively impact the other. Studies have also shown that a coordinated contraction across various sections of diaphragm is absent in patients with chronic low back pain during body movements that demand spinal stabilization.
Various studies have reported a significant correlation between low back pain and breathing dysfunction. A breathing dysfunction refers to altered breathing patterns which include simple upper chest breathing to hyperventilation. An altered respiration can alter the respiratory chemistry and thus can also influence the tissue oxygenation and electrolyte balance altering body functions including brain and skeletal muscles. Several studies have reported improved function in short term follow-ups with breathing exercises in chronic lower back pain patients.
Signs of dysfunctional breathing
Breathing pattern dysfunctions may be present along with chronic back pain if you experience symptoms like restlessness, frequent sighing, poor breath-holding times, poor expansion of lower thorax on inhalation, rise of shoulders on inhalation, rapid breathing rate or difficulty with abdominal breathing.
A few strategies to correct your breathing pattern
- Correcting an upper chest breathing pattern: Start with a lying position with one hand on the chest and the other over the stomach. Take a deep breath in through the nose, ensuring the stomach rises first (not the chest). Repeat 5-10 slow breaths per minute for 5 minutes each day.
- Gradually try the above in other static positions such as sitting and standing and progress further by integrating diaphragmatic breathing into your daily tasks and exercises.
- Most over-breathing involves too much in-breath and not enough out-breath which leads to not fully releasing the inspired air. Try breathing-in for a count of 3 and breathing out for a count of 5.
- Allow a short pause between each breath.
- Following an out-breath don’t reach for the next in-breath, rather simply allow the body to initiate it to come.
- Use a mirror to correct any unwanted movements and muscle activation of the upper chest and neck.
- Avoid negative thoughts about breathing or anything that can lead to anxiety.
References
Lise Hestbaek, Charlotte Leboeuf-Yde, Claus Manniche, DrMedScc . Is low back pain part of a general health pattern or is it a separate and distinctive entity? A critical literature review of comorbidity with low back pain. J Manipulative Physiol Ther. 2003 May; 26(4):243-52. (2A)
Kolar P, Sulc J, Kyncl M, et al. Postural function of the diaphragm in persons with and without chronic low back pain. Journal of Orthopedic and Sports Physical Therapy. 2012; 42 (4): 352-62.
McLaughlin L., Goldsmith, C., Coleman, K. Breathing Evaluation and retraining as an adjunct to manual therapy. Manual Therapy 16 (2011) 51-52
McLaughlin L. Breathing Evaluation and Retraining in Manual Therapy. JBMT 2009; 13:276-282
Beeckmans et al. “The presence of respiratory disorders in individuals with low back pain: A systematic review”, Manual Therapy. 2016; Vol 26, pag 77–86.
Hestbaek L1, Leboeuf-Yde C, Manniche C. Is low back pain part of a general health pattern or is it a separate and distinctive entity? A critical literature review of comorbidity with low back pain, J Manipulative Physiol Ther. 2003 May;26(4):243-52.
Low Back Pain and Breathing Pattern Disorders. (n.d.). Retrieved from https://www.physio-pedia.com/Low_Back_Pain_and_Breathing_Pattern_Disorders#cite_note-18